 A month ago today, I went under anesthesia for what is misleadingly classified as a minor surgery to try to get to the bottom of abnormal bleeding from my lady parts. In between two trips and pre-op appointments with both my gynecological surgeon and my primary care doctor, I spent most of October preparing for a surgery that I suspected would affect me more than the average bear, as most procedures tend to do. Living with multiple chronic illnesses that affect my immunity, pain and fatigue levels, I knew it was smart to go in prepared for the worst, but hoping for the best. I am so grateful that I took precautions, as it has only been the last couple days where I’ve really started to feel back to normal again.
A month ago today, I went under anesthesia for what is misleadingly classified as a minor surgery to try to get to the bottom of abnormal bleeding from my lady parts. In between two trips and pre-op appointments with both my gynecological surgeon and my primary care doctor, I spent most of October preparing for a surgery that I suspected would affect me more than the average bear, as most procedures tend to do. Living with multiple chronic illnesses that affect my immunity, pain and fatigue levels, I knew it was smart to go in prepared for the worst, but hoping for the best. I am so grateful that I took precautions, as it has only been the last couple days where I’ve really started to feel back to normal again.
Rooting Out the Cause of Abnormal Uterine Bleeding With a D&C
A D&C is the acronym for dilation and curettage, which involves a surgical removal of tissue from the uterine lining. While the D&C is often performed to clear the uterine lining after a miscarriage or abortion, it also used to diagnose and treat certain uterine conditions–such as heavy or abnormal uterine bleeding, as in my case. For the last couple years, I have experienced heavier bleeding than usual, longer periods and menstruation came with frequent irregularity. Some months I would have two or even three weeks of bleeding, and there were a few months when I wouldn’t have a period at all. During those rare months where I enjoyed a respite from the (bi)monthly bleed, I was always prepared for the following month or two to be a doozy.
What was going on with my body that I never knew when or for how long I would experience bleeding? For more than a year and half, my long-time gynecologist wrote it off to switching from combined hormonal birth control, which contains both the synthetic hormones estrogen and progestin, to the progestin-only birth control mini pill called norethindrone (or Micronor). I kept reminding him I had been on the mini pill for much longer than I’d observed the more significant changes in my monthly flow. I went from a few days of extra spotting to multiple weeklong flows per month. Honestly, I just wanted the old pill with its brief, light periods that occurred like clockwork. Yet the switch was necessitated by finally being formally diagnosed with antiphospholipid antibody syndrome (APS).
The Anomalies of Antiphospholipid Syndrome
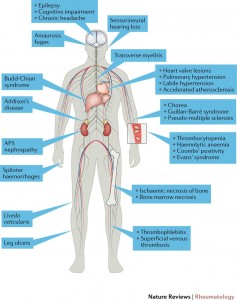 APS is an autoimmune disorder in which the body erroneously identifies certain blood proteins that bind to phospholipids – fatty molecules that comprise normal cell membranes – as foreign invaders and forms self-reactive antibodies, or autoantibodies, that attack healthy tissue. This results in difficulties control blood clotting. As a result, people with antiphospholipid antibodies are at greater risk for miscarriage, pre-eclampsia and eclampsia, as well as for developing blood blots in the veins, leading to conditions like deep vein thrombosis, pulmonary embolism; in the arteries, causing heart attacks, strokes and transient ischemic attacks (TIAs), known colloquially as mini-strokes; and, more rarely, in the small vessels of multiple organs, such as the heart, brain, kidney and/or lungs. The latter is known as Catastrophic APS.
APS is an autoimmune disorder in which the body erroneously identifies certain blood proteins that bind to phospholipids – fatty molecules that comprise normal cell membranes – as foreign invaders and forms self-reactive antibodies, or autoantibodies, that attack healthy tissue. This results in difficulties control blood clotting. As a result, people with antiphospholipid antibodies are at greater risk for miscarriage, pre-eclampsia and eclampsia, as well as for developing blood blots in the veins, leading to conditions like deep vein thrombosis, pulmonary embolism; in the arteries, causing heart attacks, strokes and transient ischemic attacks (TIAs), known colloquially as mini-strokes; and, more rarely, in the small vessels of multiple organs, such as the heart, brain, kidney and/or lungs. The latter is known as Catastrophic APS.
While I had never had been formally diagnosed with a blood clot or miscarriage (as I’ve never been pregnant), I had experienced a loss of peripheral vision following elevated thrombotic marker levels, which are often indicative of a clot in a blood vessel. At that time, I was also experiencing severe migraine headaches, mental confusion and other neurological symptoms. I got off birth control pills entirely for about six months and temporarily felt noticeably better. But as I returned to the pill, old symptoms flared and new complications began.
My head MRIs displayed brain abnormalities. The migraines continued. More distinctive rheumatological symptoms developed–joint pain and stiffness increased, rashes developed and a painful cyst grew until in needed to be surgically removed from my finger; surrounding tissue revealed a rheumatoid-like nodule. And over the next couple years, constant muscle spasms shifted into full-blown dystonia, a neurological disorder characterized by abnormal movements and postures, due to extended, involuntary contractions of the muscles. All this paired with the telltale symptoms of the blotchy, lacy rash called livedo reticularis, persistently high ANA (antinuclear antibodies) levels and a tentative diagnosis of lupus led my rheumatologist to test me specifically for antiphospholipid antibodies. When I tested positive for anti-cardiolipin, anti-beta 2 glycoprotein and more, related antibodies in blood work several months apart, the APS specialist I was now seeing confirmed my diagnosis.
Birth Control Pills, Blood Clots and Bleeding Complications
It took more than five years to get properly diagnosed after what had been, at that time, a decade of autoimmune symptoms and abnormal blood tests. Once I did, I was told to stay on Plaquenil, start taking baby aspirin daily (“for the rest of my life”) and to immediately get off of estrogen-containing birth control, as it increased my risk for blood clots even more because I had APS. Other treatments were also attempted to get better control of my increasingly disabling symptoms.
After half a year on prednisone and two years of chemotherapy treatments, I decided I needed to back off the more toxic medications and began to seek more holistic treatments, including acupuncture, massage, nutritional therapy and yoga. Eventually, my blood levels began to normalize, and I had more strength, energy and control over my pain and abnormal muscle movements. However, my gynecologist insisted I stay the course on the mini pill to reduce the risk of blood clots.
Unfortunately, the switch of birth control pills meant that I began to develop heavier, longer periods that grew more irregular over time. My doctor thought perhaps I was over-exaggerating after the first year of worsened periods, so I kept track of every bleeding day for the next year. This past summer when I went in for annual gynecological exam, he saw my calendar saturated in red circles and recognized that I spoke the truth, but he blamed the mini pill and basically told me I’d just have to deal–or switch to another hormonal birth control that probably wouldn’t make things much better.
A month or so later, when I went to my primary care physician for a suspected bladder infection, she decided to do a pelvic exam, and I wound up gushing all over her, the examining table and floor. She sent me immediately to the gynecologist. My doctor’s female partner saw me at that time and order a transvaginal ultrasound. There were the expected cysts,which I’ve struggled with on-and-off since I was 13, and a small fibroid that had nearly doubled in size from the previous year. While everyone assured me the fibroid was still quite small and was not in a position where it should cause pain, I still was feeling increasing discomfort and dis-ease. In my gut, I knew something wasn’t right.
Ruling Out Uterine Abnormalities With D&C
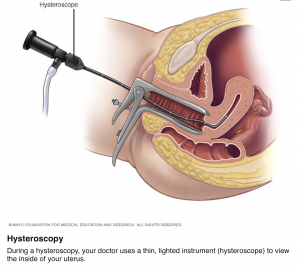
Src: MAYO FOUNDATION FOR MEDICAL EDUCATION AND RESEARCH
To be on the safe side, the female gynecologist attempted to do a uterine biopsy, right then and there, to help rule out uterine fibroids, polyps or even cancer. But due my petite size, the procedure caused tremendous pain and discomfort. I’d already had a vasovagal syncope episode during an attempt to place a progestin-containing IUD in the uterus a couple years earlier. At that time my face “turned green” according to the doctor, and I felt nauseated, lightheaded, clammy and was seriously at risk of fainting for quite some time afterward. This new doctor didn’t want to risk causing another episode, so quickly stopped the biopsy attempt.
When I had a followup with my regular gynecologist a week or two later, he decided the best bet for getting a real look at what was really going on inside my pelvis was to perform a D&C with a diagnostic hysteroscopy in the hospital, where I could be carefully monitored for bleeding complications that might result from having APS. A simple, in-office procedure suddenly became a more complicated surgery in the hospital. Blood needed to be made available for a possible transfusion. I would wear compression boots, or intermittent pneumatic compression devices on my legs, to massage them to increase blood flow and prevent deep vein thrombosis (DVT) blood clots from forming. I was asked multiple times if I had a living will. Both my husband and my parents took time to be there during the surgery and help in recovery.
I was given the medication misoprostol (Cytotec) to take the night before my procedure to dilate (open) and soften the cervix so that the doctor could use a surgical instrument called the curette to remove uterine tissue for endometrial sampling. I bathed myself in surgeon-approved antibacterial soap. I put on my baggy sweats that I’d bought two days before surgery. I had my prescribed anti-nausea medication on hand.
As the surgical team prepped me for the procedure on that Friday morning four weeks ago, my husband and I had to explain to them what dystonia really was as they observed periods where I couldn’t communicate verbally because my mouth, jaw and neck were twisting harshly. A wheelchair was procured to bring me into the operating room. A nurse (coincidentally who also has APS) attempted to stab my hand for the intravenous needle. Only succeeding in causing excruciating pain, she finally found a good vein opposite my elbow, like I’d originally suggested. I tried to regain my composure with several meditative breaths,
Due to the complications of the health conditions I have, the multiple medications I take for them, and the technical simplicity of the surgery, my gynecologist and the anesthesiologist agreed that it would be best if I did not go under full, general anesthesia as originally posited. The twilight anesthesia technique was instead used to decrease my level of consciousness, to cause anterograde amnesia and to block pain by intravenously giving me the medications Propofol and Fentanyl. In other words, while I was not technically unconscious, I had no awareness or physical sensation of the procedure while it was going on, and I woke up with no memory of what had just been done to me.
I was stunned to return to full awareness just 15 minutes after the mask was put over my mouth. I remember being instructed to put my feet in the stirrups and to position my head and tailbone just so on the small, firm cushions. My doctor announced from somewhere between my legs that they would have to cut off the granny underwear they had given me to wear after I’d announced that I was (of course) still bleeding. And suddenly, there was nothing.
The Bumpy Road To Recovery After A D&C
 And just as suddenly again, a nurse was smiling at me and talking gently until I could once again respond. My doctor came out and told me things had gone very well, with no complications. He noted that my uterine lining was quite thin. The normal course for that was to build up my endometrial layer with estrogen, but of course we couldn’t use, but we’d talk about that later, he promised.
And just as suddenly again, a nurse was smiling at me and talking gently until I could once again respond. My doctor came out and told me things had gone very well, with no complications. He noted that my uterine lining was quite thin. The normal course for that was to build up my endometrial layer with estrogen, but of course we couldn’t use, but we’d talk about that later, he promised.
Before I knew it, I was home. After the medication wore off, there was the expected cramping, spotting, nausea and abdominal pressure. It took several days before I could be in a bending position without severe pain. However, I did gentle stretches and bed yoga as soon as I was able. By the end of the week, I was pretty much back on my feet with a slightly modified version of my normal daily practice.
Unfortunately, the painful abdominal pressure and bloating that developed post-surgery never fully went away. When I went in for my post-op appointment with the certified physician assistant, she said she suspected I had developed a bacterial infection. It was then confirmed by lab test. Even during a week of antibiotics, the abdominal discomfort and pelvic pain were so severe, it hurt to be touched anywhere on my abdominal area, and I couldn’t wear any pants that put even the slightest pressure on my belly. Eating seemed to make it worse. Fasting seemed to make it worse. Pooping certainly didn’t make it better. Staying still was already uncomfortable, so I just kept moving as I was able, even getting unexpected lost in the woods on what became an extended hike.
A week ago today, the last day of antibiotics, my symptoms seemed no better, and I was spotting again. There were signs that my period was trying to start, but something seemed to be preventing the flow. I had my annual physical exam with my primary care doctor that day. After a complicated hour-and-a-half visit that included an EKG (or electrocardiogram), my doctor made me promise to get into see the gynecologist that day.
A few hours later, I was back in the office with the physician’s assistant. This time she seemed to poo poo (pardon the pun) my symptoms as just gas. I assured her it was different from gaseous bloat – I was having regular bowel movements (far more frequent and productive than usual for me, in fact). The abdominal pains I experienced were above and beyond the pelvic pain from cysts that I typically felt forming around my period. But, of course, my ridiculously inflated belly had decreased by this second visit. An acupuncture appointment the previous day had relieved some of the tenderness. But I believe a brief burst of blood flow between Friday’s doctors visits helped deflate the beach ball in my stomach. While I was back to stopped up in the stirrups, an ultrasound was ordered, nonetheless. Unfortunately, the ultrasound tech was booked for the rest of the afternoon. I was given the option of returning the following Monday late afternoon, but the timing was inconvenient, so I agreed to push out until the following Wednesday, after Thanksgiving.
A sushi dinner that night needed to be halted when I felt the pain, pressure and inflation fully returned. A couple days later, my period finally came in earnest, and I started to feel longer-term relief. The bloating went down, the abdominal pain decreased, and I have been left with a strong, long and heavier than normal period ever since. It’s kind of opposite of what I was told to expect after the D&C, but that honestly hasn’t surprised me.
The good news, though, is that even after a hearty consumption of two Thanksgiving dinners (the husband and I always head to both sets of parents each holiday), I could wear normal jeans without my belly blowing up and over the waistline, and I was surprisingly without any sharp pains in the abdomen. That morning, I could clearly see my abs once again without flexing too. The jury is still out on whether this relief will last, but I am grateful for this respite, at least.
The Road to Ditching The Birth Control Pill
 My journey is not over, however. After a couple months of research on the seriously negative side effects of long-term hormonal birth control use, my husband and I are fairly convinced that I should go off the birth control pill as soon as my doctor gives the okay. I was urged to wait three months to give a honest assessment of whether the D&C was beneficial or not; I visit my gynecologist again in February. For me, it’s not question of if I’ll get off the pill, but when I will.
My journey is not over, however. After a couple months of research on the seriously negative side effects of long-term hormonal birth control use, my husband and I are fairly convinced that I should go off the birth control pill as soon as my doctor gives the okay. I was urged to wait three months to give a honest assessment of whether the D&C was beneficial or not; I visit my gynecologist again in February. For me, it’s not question of if I’ll get off the pill, but when I will.
I’ve heard and read enough testimonials of women who’ve gone off the pill – by both experts and personal friends – to consider this weaning the next major chapter of my healing path. The fact that I have actually had a simulated period for the vast majority of the last two decades is mind-boggling. Thanks to synthetic hormones, monthly bleeding for women on hormonal birth control pill is actually due to medicinal withdrawal, not from bona fide menstruation. And for those of who get the same dose of the synthetic hormone progestin throughout the month on the mini pill, the body seems to get even more chaotic and confused, which results in this increased bleeding. With this type of hormonal dysregulation for years and years on end, it’s no wonder so many women these days are so out of touch with our own bodies and nature, right?
So I’m stoked to do a full withdrawal from synthetic hormones and to return to my body’s natural rhythms. According to Sweetening the Pill by Holly Grigg-Spall, the reproductive “hormone cycle regulates 150 bodily systems all of which are suppressed by hormonal contraceptives and all of which are related to all other body symptoms (including endocrine, neurologic and immunologic systems).” In other words, the ebbs and flows of the female reproductive system is intrinsically intertwined with the natural rhythms of of the human body as a whole.
These rhythms of the human body are meant to be reflective of the ebbs and flow of nature. My body, mind and spirit are naturally aligned with the cyclical flow and creative force of the Universe. Shara Vana Ya. And so it shall be.
I hope you continue on your road of healing and recovery! I’m very familiar with the first-hand frustrations that arise from APS and mentrual cycles. I also have Sjogrens too. I am on a similar path of healing and many days it’s very exhausting. APS can be tough because there are so many strange side effects, but honestly the best thing I’ve found is movement and healthy eating- as well as my prescription medication. I do not think it’s safe to be on any birth control at all once APS is diagnosed. I did try an IUD- which my body painfully rejected and pushed into my uterine lining causing intense bloating and severe pain. Good luck on your path!!!!
Thanks so much for sharing some of your story, Erica. I know having both APS and Sjogren’s must make life utterly exhausting and overwhelming at times. I think you’re right that it’s not the safest to be on any type of hormonal birth control with APS, and I can’t wait to get off it shortly. Your IUD experience sounds like a nightmare What type of movement and which medication have you found work best for you?
What type of movement and which medication have you found work best for you?