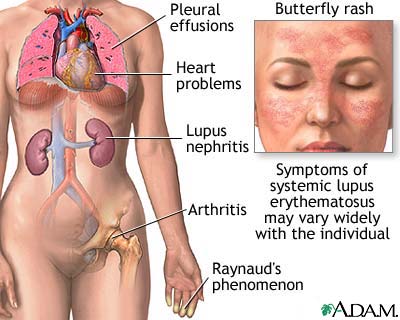
 In autoimmune diseases like lupus and rheumatoid arthritis (RA), the immune system misfires by erroneously attacking healthy cells as if they were foreign agents, or antigens. Normally the immune system defends the body against antigens—like viruses, bacteria and toxins—that can cause damage to the body after invading it. In autoimmune diseases, benign and healthy parts of the body also become victims. Therefore, when autoimmune disease is systemic, affecting the entire body, it has the potential to attack the joints and organs of the body—including the skin, kidneys, lungs and heart.
In autoimmune diseases like lupus and rheumatoid arthritis (RA), the immune system misfires by erroneously attacking healthy cells as if they were foreign agents, or antigens. Normally the immune system defends the body against antigens—like viruses, bacteria and toxins—that can cause damage to the body after invading it. In autoimmune diseases, benign and healthy parts of the body also become victims. Therefore, when autoimmune disease is systemic, affecting the entire body, it has the potential to attack the joints and organs of the body—including the skin, kidneys, lungs and heart.
Lupus and RA can cause inflammation of the heart muscle, arteries or the lining of the heart (the pericardium), as well as abnormal heart rhythms. People with the inflammation of these autoimmune diseases are thus at greater risk for developing cardiovascular disease or suffering from strokes.
In 2012, Karen Costenbader, MD, MPH–a rheumatologist who co-directs the Lupus Center at the Brigham and Women’s Hospital in Boston, Mass.–and two colleagues performed a review of 28 studies analyzing the association between lupus and heart disease. They found strong evidence for people with lupus having at least a twice to three times the risk of developing heart disease and stroke, compared to those without lupus. For those under age 45, people with lupus also had a significantly higher risk for these cardiovascular events.
Researchers at the University of Arkansas for Medical Sciences also found that people with lupus and RA have a greater risk for developing the heart condition linked with stroke, atrial fibrillation (AF).
According to U.S. News, a 2011 study found that patients with lupus or RA were 1.6 times more likely to have atrial affribrilation than people without these autoimmune disease. A study of 416,786 American patients older than age 65 treated for AF revealed those with autoimmune disease had a 60 percent increased risk of developing the heart condition.
Atrial fibrillation (also known as afib) is an electrical disorder of the upper chambers of the heart that causes arrhythmia, or abnormal heart rhythm. Having afib increases the risk of heart-related problems and stroke. As it tends to affect a greater number of older adults, an aging population has seen a sharp increase in afib diagnoses. Yet due to potential involvement of the heart, blood vessels and clotting mechanisms, people living with lupus and sister condition antiphospholipid antibody syndrome have a greater risk of developing heart disease at an early age.
Lupus Foundation of America, states the approximately 1.5 million people living in the U.S. have lupus, and the Arthritis Foundation estimates that 1.3 million have RA. According to the Cleveland Clinic, more than two million Americans have afib.
Healthline.com offers a more in-depth explanation of Afib:
 The Effects of Afib on the Body
The Effects of Afib on the Body
Afib affects the upper chambers of the heart, called the atria. It’s an electrical disorder that causes rapid electrical signals in the heart that may reach hundreds of beats per minute. The rapid-fire signals interfere with the ability of the upper chambers to contract in an organized way.
This leads to decreased pumping action and passive blood flow. Blood can even pool within the heart. Some people with afib have no symptoms, while others experience a wide range of symptoms. Afib increases the risk of heart-related disorders and stroke.
 Circulatory System
Circulatory System
When the heart’s electrical system is out of whack, the heart chambers lose their rhythm. A common symptom of afib is the sensation that your heart is flopping around inside your chest, or simply beating irregularly (palpitations). You may become hyper-aware of your own heartbeat.
Over time, afib can cause the heart to weaken and malfunction. The heart’s ineffective contractions cause blood to pool in the atria. This can increase the risk of clotting. As a result, you may experience shortness of breath, low blood pressure, and chest pain. During an episode of afib, your pulse may feel like its racing, beating too slowly, or beating irregularly.
Heart failure occurs when the heart loses its ability to circulate enough blood throughout the body.
 Central Nervous System
Central Nervous System
Afib increases the risk of stroke. When the heart fails to contract properly, blood tends to pool in the atria. This increases the risk of forming a clot. When the heart pumps, the clot can travel to the brain, where it blocks the blood supply and causes an embolic stroke.
Early warning signs of stroke include severe headache and slurred speech. If you have afib, your risk of stroke increases as you age. Other additional risk factors for stroke include diabetes, high blood pressure, or history of other heart problems or previous stroke. Blood thinners and other medications can lower that risk.
 Respiratory System
Respiratory System
The lungs require a steady supply of blood in order to function properly. Irregular pumping action of the heart can also cause fluid to back up in the lungs. Symptoms include shortness of breath, difficulty performing physical activities, and fatigue.
General Health
Some people with afib may have a build-up of fluid in the legs, ankles, and feet. Other symptoms include weight gain, lightheadedness, and a general sense of malaise. Some patients report irritability and exertion during previously routine activities.
Healthline Sources:
- Atrial fibrillation or flutter. (2013, May 3).MedlinePlus, National Institutes of Health.Retrieved December 12, 2013 fromhttp://www.nlm.nih.gov/medlineplus/ency/article/000184.htm
- Drs. Lindsay, Van Wagoner, and Gillinov. (2011, June 13). Atrial fibrillation. Cleveland Clinic. Retrieved December 12, 2013 from http://my.clevelandclinic.org/heart/webchat/1271_atrial-fibrillation.aspx
- Atrial fibrillation. (n.d.). Stanford Hospital & Clinic. Retrieved December 12, 2013 from http://stanfordhospital.org/cardiovascularhealth/arrhythmia/conditions/atrial-fibrillation.html

Leave a Reply