Cynthia Toussaint was a promising, 21-year-old ballerina when she was struck by a seemingly simple hamstring injury that ultimately led to a lifetime of widespread pain. After being a performer for so many years, Toussaint was accustomed to the bright lights and action of the stage. Now she would have to learn to manage the burning heat and immobility of chronic pain.
“I had just had gotten a role on the TV show Fame when I was struck with CRPS,” Toussaint said in a recent interview.
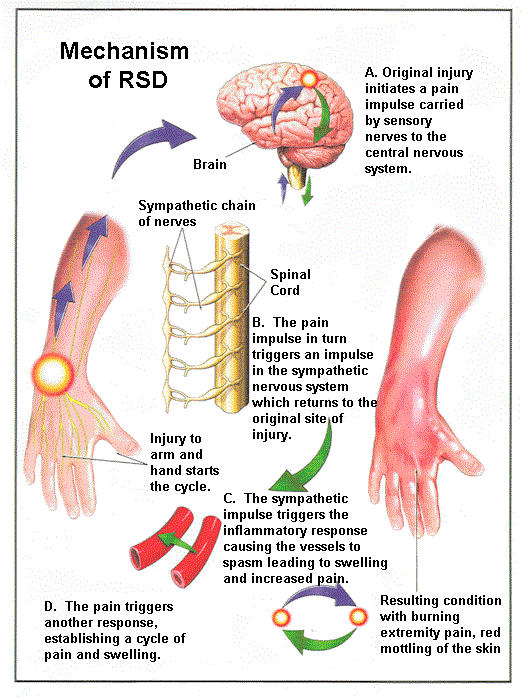
Complex Regional Pain Syndrome (CRPS) is a chronic pain condition believed to be cause by damage to or malfunction of the peripheral and central nervous symptoms. Formerly known as Reflex Sympathetic Dystrophy (RSD), the neurological condition is characterized a constant burning pain, inflammation of tissues and affected joints, contractions of the blood vessels (vasoconstriction) and muscles of the extremities (spasms), and changes in skin color, texture and temperature. People with CRPS may also have motor dysfunction (including dystonia), excessive sweating and extreme sensitivity to temperature, sound, vibration and touch.
“[CRPS] is a message that goes to the brain that sends, ‘pain, pain, pain,’ and it amplifies and does not know how to shut itself off,” Toussaint, now 52, explains. “And the pain feels as though my body has been doused with gasoline and lit on fire.”
Despite the excruciating pain of CRPS, Touissant continued to dance for as long as she was able. “After I got ill, I first got a job dancing in Reno, then Vegas, and I stayed with that act because I wasn’t going to lose my life as long as I could,” she said. “And finally the disease spread from my right leg into my left, and I could no longer fake it.”
 Undiagnosed for 13 years, Touissant was told her symptoms were “all in her head.” Meanwhile, her condition worsened and left her bedridden for a decade. “I was unable to speak while the disease spread throughout my entire body and ravaged my vocal chords,” she said.
Undiagnosed for 13 years, Touissant was told her symptoms were “all in her head.” Meanwhile, her condition worsened and left her bedridden for a decade. “I was unable to speak while the disease spread throughout my entire body and ravaged my vocal chords,” she said.
CRPS is known as a suicide disease, Touissant said, and she is familiar with the desire to permanently escape the incessant pain. “I realize now, looking back, that it was my coping mechanism because we have to have a way out. The pain is so excruciating, and you lose your career, everybody leaves you, and the doctors say you’re crazy,” she said.
“It’s really an unlivable situation, and having this incredible man stick by me and believe me when nobody else did,” Cynthia said, reaching out to grasp her husband’s arm. “I can say safely that not only would I not be here if not for opiods that have saved me, but also I would not be here if not for John.”
John Garrett has been Cynthia’s loving caregiver for the last 32 years. He stresses the importance of bearing witness to those suffering with chronic pain. “The first thing to do is to believe them and trust what they’re telling you is really what’s going on,” he said. “Because chronic pain is a real bear to have to bare through—there’s no doubt about it. It’s a challenge on so many levels. So you want to just believe them, you want to trust them, you want to honor them and embrace them for the experience they’re going through and try to help them through a very, very, very difficult situation. But it’s something to give a lot of love to, for sure.”
Toussaint was finally diagnosed with CRPS in 1995, along with the overlapping condition fibromyalgia. Since then, she has experienced significant improvement and moved from the bed into a wheelchair. She is presently experiencing her first partial CRPS remission in 32 years and can now swim a mile.
“I can swim a mile but I can’t walk a block,” Toussaint quipped.
She credits her improvement to multiple factors, including firing her conventional doctor and writing her own story in the memoir, Battle for Grace: A Memoir of Pain, Redemption and Impossible Love. “I think honestly I stopped going to doctors who were actually making me a lot worse, and I wrote my book,” she said “And I think it was the narrative therapy of writing my book and going to an alternative therapy doctor that helped me.”
[youtube https://www.youtube.com/watch?v=9trhl-1wMhg]
Toussaint receives acupuncture, trigger point injections and acupuncture from her new holistic doctor. She also takes a proactive role in her own healing by eating a healthy diet, staying hydrated and practicing good sleep hygiene. “I also do meditation every day,” she said. “Lots of self-care.”
Opioids have also played a critical role in helping Cynthia manage her CPRS. “For me, after being bedridden for 10 years and finally getting my diagnosis after 13 years I learned that opioids were an excellent and effective way for me to manage my pain,” she said. “However, I do deal with this very serious side effect known as OIC. It can be very severe.”
OIC, or opioid-induced constipation, is a serious side effect of taking opioids. For Toussaint, OIC resulted in a hiatal hernia after consistent straining. This straining also exacerbates her CRPS pain.
“On my—our—OIC days, very often my walking is either very limited, or I can’t walk at all, in which case John has to literally be my legs not only for my work and everyday chores, but also he literally has to get me to and from the bathroom time and time again or bring the bathroom to me,” she said. “So it’s really a supreme challenge, living with OIC.”
While Cynthia must sometimes rely on Garrett to “be her legs,” she describes herself as a very independent person who uses her wheelchair whenever she can. She counsels otherwise self-reliant people with chronic pain to just honestly ask for help when they need it. “I’ve gotten very good at asking and sort of demanding. I sort of give John orders—I have to admit—at this point,” she said.
Her husband seems to take the added responsibilities in stride. “It always gives me a great opportunity to put my arms around her, which is not such a bad thing, you know?” he said.
On a more serious note, Garrett recognizes how stressful and energy-consuming being a caregiver can be. He notes how easy it is for people in chronic, long-term caregiver situations especially to lose themselves, giving up their own dreams, ambitions and goals. He urges loved ones to find ways to carve out time for themselves and their own pursuits as well.
“I mean you want to give so much love. You want to take care of this person, and so often, you give up on yourself in some respects.” Garrett advises, “Yeah, you love that person and take care of them, but, you know, love yourself, take care of yourself too, and hold onto those dreams and passions that you have.”
One of the passions that Cynthia and John share is promoting better care and wellness for women in pain, which is what they accomplish with For Grace, the nonprofit they founded more than 12 years ago. With more than 100 million adults in America with chronic pain, the couple believes it is important to offer help and valuable information through their website www.forgrace.org, public speaking and caregiver support groups.
They have also gotten involved with legislation, most notably with the Assembly Bill 889 to reform the Step Therapy, or “fail first,” prescription practice. Step Therapy requires a patient to “fail” on up to five different medications before being allowed to have the one originally prescribed by his or her physician.
“This is an unethical prescription practice that the health insurance industry uses at the cost of the paying patients,” said Toussaint, who recently spoke on Capitol Hill. “We did get it to Gov. Brown, our California governor’s desk, a couple of year ago, and he vetoed it. And we’re plowing on through. We never quit. We won’t stop until we get it signed.”
[vimeo 79492261 w=500 h=281]
Pain Matters from Discovery Channel CME on Vimeo.
For Grace is also committed to bringing light to the disparity of health care women face in the assessment and treatment of pain conditions. Its Women in Pain Awareness and Education Project helps to educate the public about gender disparities in pain management—women are more often under-treated for their pain, to inform and empower women to become better advocates for their health, and to enlighten policymakers about the major national health crisis of chronic pain.
According to a 2011 report, Relieving Pain in America: A Blueprint for Transforming Prevention, Care, Education, and Research, by the Institute of Medicine, the public health crisis of pain costs the nation more than $560 billion annually, including rising medical expenses and lost productivity and wages. When children and military personnel are included, these numbers rise significantly.
It is estimated that at least one-third of the American population live with chronic pain today, more than the number of people living with cancer, heart disease and diabetes combined. Pain is cited as the number one complaint for patients seeking medical attention in the country. Chronic pain is medically defined as any pain in the body that lasts more than three months.
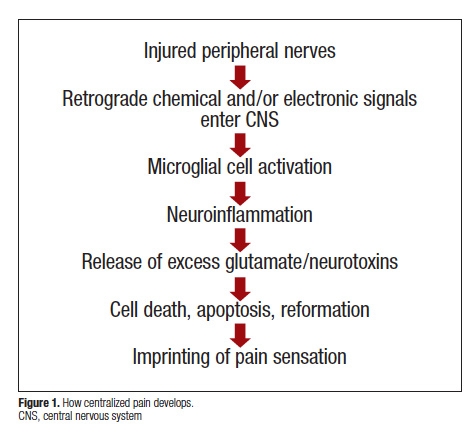 When a peripheral injury doesn’t completely heal, chronic pain can cause structural, functional and chemical changes in the brain, altering how it processes and modulate pain signals. The brain begins to generate abnormal levels of excitatory and inhibitory neurotransmitters–chemicals that relay signals between nerve cells, communicating information through the brain and body. Due to abnormal function in brain circuitry, chronic pain may also hinder autonomic responses and cognition, affecting memory and emotions. A constantly inflamed and hyperexcitable central nervous system caused by the now centralized pain can result in allodynia (pain to light touch), hyperalgesia (excess pain on pressure), as well as dysfunction in hormone production, tachycardia (abnormally fast heart rate), hypertension (high blood pressure) and vasoconstriction (cold hands and feet) and insomnia. What starts as a focal injury may easily become systemic and increasingly complicated to manage and treat.
When a peripheral injury doesn’t completely heal, chronic pain can cause structural, functional and chemical changes in the brain, altering how it processes and modulate pain signals. The brain begins to generate abnormal levels of excitatory and inhibitory neurotransmitters–chemicals that relay signals between nerve cells, communicating information through the brain and body. Due to abnormal function in brain circuitry, chronic pain may also hinder autonomic responses and cognition, affecting memory and emotions. A constantly inflamed and hyperexcitable central nervous system caused by the now centralized pain can result in allodynia (pain to light touch), hyperalgesia (excess pain on pressure), as well as dysfunction in hormone production, tachycardia (abnormally fast heart rate), hypertension (high blood pressure) and vasoconstriction (cold hands and feet) and insomnia. What starts as a focal injury may easily become systemic and increasingly complicated to manage and treat.
Earlier this month, the National Institutes of Health (NIH) published a report citing the insufficient options for effective treatment of chronic pain beyond opioids. The report cited an increasing need for research into better treatment methods and improved physician education and preparation for managing chronic pain. According to TIME, the NIH said that complementary and alternative medicine should be considered favorable pain treatment options, in addition to physical therapy. With both physical and emotional components to chronic pain, the NIH advises a multi-disciplinary approach and individualized treatment for chronic pain.

I’ve had RSD from surgery from a work injury since 2004, I was 35. It’s so very hard to continue being strong emotionally. I have found the love of my life, and he’s been with me 6 1/2 yrs. My RSD is local yet, I’m facing surgery in the opposite shoulder same issue. This is a fantastic story. I’m so happy you found a good doc to help you!
Thanks so much for reading and commenting. It’s definitely difficult to stay strong through such a harrowing condition. So glad you have loving support. Best of luck with the surgery!
My daughter has the same condition and has lost both legs because of it. She is trying to get the health service in the uk to get this dreadful and debilitating condition researched. She too has had the “it’s all in your head” statement. My daughter has also started. to write her story and has her own website chronicpaincrps.com. As a family we are determined to get this syndrome into the research world.
I’m so sorry to hear about your daughter’s losses to CRPS. She is so blessed to have you and your family’s support and love. We desperately need more research AND validation from the medical community on chronic pain syndromes, such as this one. I will definitely read her story on ChronicPainCRPS.com. Perhaps she might want to contribute a guest post here?
Reblogged this on .
Thanks so much for sharing this article!
You are so very welcome! I also have RSD/CRPS and spend the majority of my time in bed as it hurts too much to try and put pressure on my feet. That is where I am affected, both feet. The story gave me a glimmer of hope about my deteriorating condition. xoxo Lysa
You are so very welcome! I also have RSD/CRPS and spend the majority of my time in bed as it hurts too much to try
and put pressure on my feet. That is where I am affected, both feet. The story gave me a glimmer of hope about my deteriorating condition. xoxo Lysa
Lysa, so glad Cynthia’s story touched and encouraged you! That’s why I felt so compelled to write about her. I know the frustrations of spending your life in bed due to pain, amd I pray you are able to find ways to better manage the disease so that you too can see improvement.
Thank you so very much for the well wishes! I was able to somewhat function for a few years but the past six months I have just been getting progressively worse… I plan to see another NEW Dr. in a few weeks so I pray there will be something they can do for me! Wishing you a fabulous afternoon!
Much love,
Lysa
Lysa, I’m so sorry to hear about the deterioration of your CRPS. I wish you the absolute best with the new doctor! Keep me updated. Best, Renée