While covering a touchy subject and including a graphic surgical graphic, I feel this is important to share, and I wish I had had something like this to read before my procedure. Hopefully it provides helpful information and even a little reassurance in the event you need a biopsy for a breast lump in the future.
A year ago, my OB-GYN or ‘lady doctor’ as I like to call him, declared that it was time for me to get a baseline mammogram, at the age of 35. After the procedure, I was informed that I have very dense breast tissue—not a surprise—so I scheduled a follow-up ultrasound. I don’t remember the specific wording of those ultrasound results, but there was a palpable mass significant enough to keep an eye on, so I was told to get another ultrasound six months later. Having dealt with the long back-and-forth of what turned out to be a benign fibrocystic breast lump in my early 20s, I figured there was no reason for concern and, unwisely, skipped the follow-up.
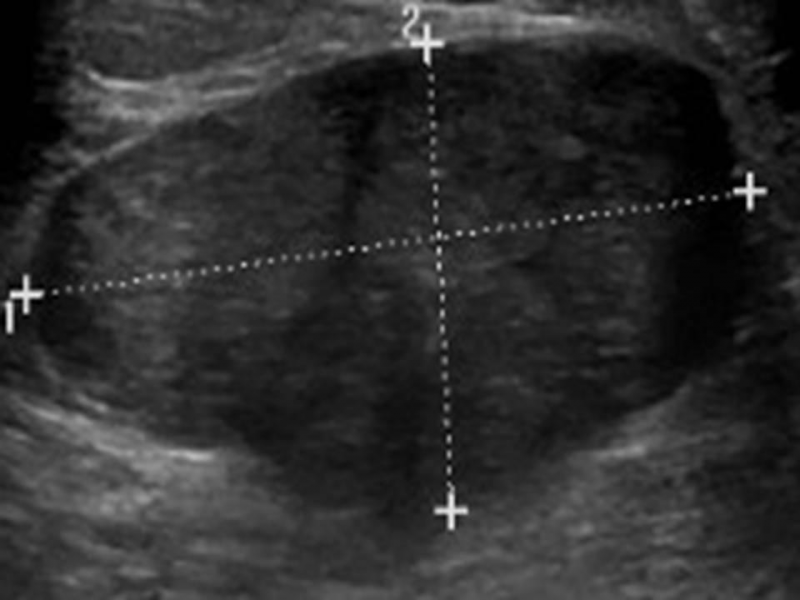
A month or two ago, after my annual “lady” exam, my doctor insisted I get the follow-up ultrasound. This time, I did, which I’m extremely grateful for, because they found the solid breast nodule, distinct from other cysts (clear, fluid-filled) in my breasts, had grown significantly in the last year. I was quickly scheduled for an appointment with a breast surgeon from a practice that came highly recommended.
When she walked into the office, the surgeon said, “You have a fibroadenoma in your breast. It’s most likely benign, but we don’t like growing things in the breast, so we’re going to remove it.” The surgery would require general anesthesia but would take a couple hours, and I’d be comfortably back home the same day.
Then, she went on to do an ultrasound and manual exam. The mass was difficult for her to find either way, which made her hesitant to do the lumpectomy. “We don’t know exactly what we’re dealing with here,” she said, “so let’s do a biopsy rather than attempt to remove what may not be a fibroadenoma.”
Being the proactive patient from years and years of practice, I looked up the different types of breast lumps, both benign and cancerous. A fibroadenoma is a solid, noncancerous breast tumor. When I got my ultrasound results, I looked up the definitions of “hypoechoic” (does not echo sound waves well), “slightly lobulated” (consisting of lobules, or milk glands), and “periareolar” (which, not surprisingly, means over the areola circle around the nipple). I checked where the size of my enlarged lump matched up with different kinds of lumps. I compared “common features” of benign breast lumps to traits of cancerous ones. In short, I tried to learn the most I could on something about which I couldn’t possibly know anything definitive.
Did it assuage my concerns? Nope. Did it lead to more questions? You bet.
From the day of getting my first ultrasound results to the appointment with the breast surgeon was almost two weeks. The biopsy was a week later. The pathology results came two days later. Some days were filled with anxiety—not knowing somehow seemed so much worse than knowing one way or the other. Other days, I packed with absorbing fun and busyness to keep my mind on the positive and joyous.
“I am okay,” I kept telling myself. “No matter what, I’m going to be just fine.” I started to believe it too!
Despite all my reading, I was not fully prepared for the biopsy once it arrived. I knew to be wearing a sports bra, but the intake nurse told me I would have to stay away from exercise for three days (what, no yoga?!), couldn’t swim for 3-5 days (this was naturally over three of the hottest days of the season), and couldn’t shower for 24 hours, which honestly wasn’t that big of a deal. None of these things I knew of beforehand, so all the info at once made me feel rather frazzled.
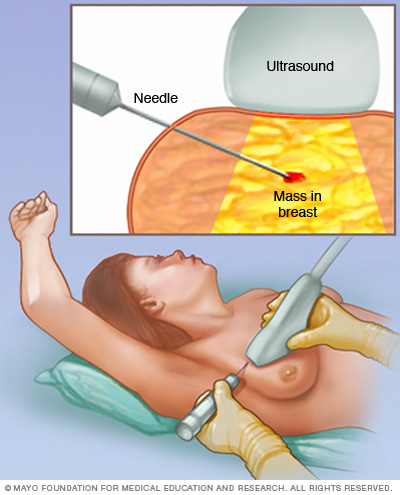
I had a core needle biopsy, where a thin hollow needle pulls out tissue samples from multiple sites on the breast—it sounded like a staple gun, but I didn’t feel a thing. My biopsy was guided by ultrasound—the mass was ill defined with “tentacles,” covering a broad area. The actual procedure was painless and not too nerve-wracking, thanks to local anesthesia of lidocaine and to my knowledgeable, reassuring radiologist and tech. What I could feel was occasional tenderness under the pressure of the ultrasound transducer, or wand. Afterwards, I had to have a mammogram.
I showered again mid-afternoon the next day. I didn’t linger long in the water—I was already worried about getting drenched in the sweltering heat from the quickly melting ice used to ward of swelling. After the shower, it was time to take off the band-aid covering Steri-Strips, adhesives used to close the small wounds from the biopsy. With all the medical procedures I’ve endured, blood doesn’t bother me much, but I was surprised by how messy the biopsy site was underneath the strips. They did wind up having to take a good number of samples. While less frequent than the previous day, I still needed to have half-hour icing sessions throughout day 2.
That night, I briefly removed my sports bra for a simple, snug, white camisole. A couple hours later, my boyfriend pointed at my chest and said, “Baby, are you okay?” It turned out the biopsy site had started actively bleeding again. In a bit of a panic, I wiped things up as delicately as I could, and put more gauze over the area, securing it with adhesive tape. It continued to bleed for a couple hours longer despite pressure with ice and a pillow. After a couple calls to doctors after-hours, I was confident I wasn’t in any danger, but I lay in a heap of throbbing discomfort on the couch all night.
The next day, I was called to come back to the radiology department, just to make sure the bleeding wasn’t due to a hematoma. The radiologist did a quick ultrasound and was pleasantly surprised to discover I did not, in fact, have a sac of blood collecting in tissue outside the blood vessels. I’ve had one before when I had all four wisdom teeth pulled out at the same time—it was extremely painful and unpleasant. The radiologist and tech also were able to see that the results from my pathology report had come in:
Benign. Thank God.
While I felt that wave of relief spreading over my body and mind, the radiologist reminded me I would get another ultrasound in six months. After that, I should not need another mammogram or ultrasound until age 40—3 years later. A tiny device was implanted during the procedure, marking the spot for future imaging of the breast, letting any medical professional know that area has already been biopsied.
“Keep doing breast self-exams,” the radiologist told me. “Just because this was benign doesn’t mean the next time you find a lump, it will be benign too.”
He said it not to scare me, but to give me a reality check. (Don’t wait a full year for follow up, next time!)
Listen to your bodies, ladies. Feel your boobies on the regular. Be preventative, not reactive—as much as you can be. Take good care of your body, ‘cause it’s the only one you’ve got.
I’m glad it is benign!
If you need a loving kick in the nether regions to remind you not to wait for followups, feel free to ping me. I have special boots for such occasions.
Thank you!
Loving kicks in the nether regions are much appreciated W!
I just had the same procedure done yesterday. Thank you for your post. It does give me a bit of comfort. I am praying for the same result. It will set your priorities in the correct order and quickly too!!
Sabrina, I pray you also had benign results. These kind of scares definitely nudge you toward reprioritizing your life. Please let me know how things turned out!